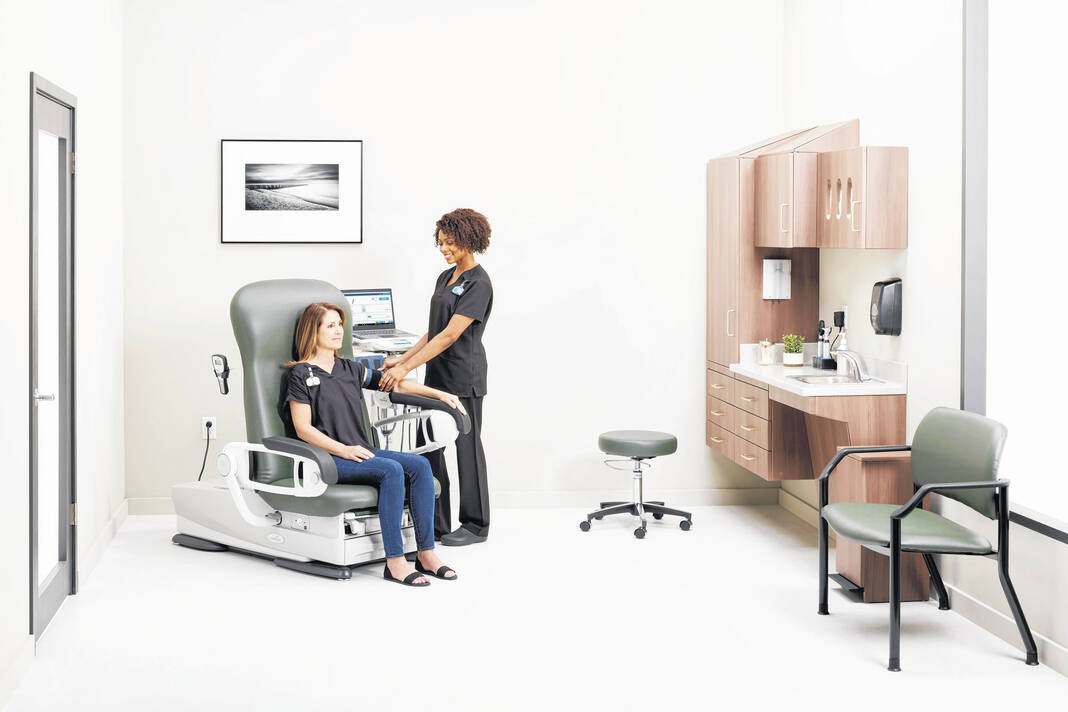
The CORRECT BP study authors and study designers chose to use the Midmark 626 Barrier-Free Examination Chair to ensure proper participant positioning following AHA recommendations.
Submitted photo
VERSAILLES — A new study on blood pressure (BP) measurement found that adhering to positioning guidelines recommended by the American Heart Association (AHA) resulted in substantially lower BP values when compared to commonly employed technique and improper positioning. A peer-reviewed report of the CORRECT BP study has been published in eClinical Medicine, part of The Lancet Discovery Science.
Key findings of the CORRECT BP study include:
* AHA-recommended positioning resulted in substantially lower BP values when compared to those readings obtained within routine clinical care where AHA-recommended positioning procedures for BP attainment were not followed.
* BP readings taken on a fixed-height exam table where the proper AHA protocol could not be achieved were significantly higher than readings taken using the proper technique with the patient seated in an exam chair with adjustable positioning options.
* Pooled systolic/diastolic BP readings taken on the exam table with incorrect positioning were markedly higher by 7.0/4.5 mmHg (both p<0.0001) than those taken in the exam chair.
* These significantly higher readings could result in misclassifying a patient as having hypertension
* The observed benefit of proper positioning is sufficient to change the classification of BP disorders for millions of patients from hypertensive to normal.
The results support estimates that as many as 30 million or more Americans may be incorrectly classified as having hypertension.
“Of all the vital signs, BP measurement has perhaps the most clinically significant connection to point of care diagnosis, patient risk stratification and proper medication dosing. Unfortunately, it also continues to be the point of care test that is most inconsistently performed in the clinical environment,” said Dr. Randell Wexler, corresponding author of the study and professor and academic vice chair, Department of Family and Community Medicine, The Ohio State University College of Medicine. “Accurate BP measurement can help reduce instances where a patient might be overmedicated, which can increase the risk of side effects that often will impact compliance with medication.”
In 2017, AHA published new guidelines for in-clinic BP measurement that largely mirrored the highly specific protocol for BP measurement defined in the SPRINT study published in the New England Journal of Medicine. Many of the known causes for avoidable variation in point of care measurement were taken into account in the SPRINT protocol, except for the known impact of white coat hypertension.
The CORRECT BP study was designed to determine the effect of poor positioning that occurs when BP is taken with the patient sitting on a typical clinical exam room table, where the feet are not flat on the floor, the back is not supported and the arm is not supported with the BP cuff at heart level.
“It is important to understand that the CORRECT BP study is not a criticism of healthcare providers’ current measurement processes. It is a reminder that even with something as seemingly simple and routine as BP measurement, there is the risk of human errors and inaccuracies occurring when proper protocols are not followed. This study demonstrated that these errors are indeed substantial and can directly impact clinical decision-making,” said Tom Schwieterman, chief medical officer and vice president of clinical affairs, Midmark.
“Through our Better BP initiative, Midmark has been offering education to healthcare providers on the importance of consistent BP capture, as well as how to take the necessary steps to ensure a more consistently accurate BP measurement process.”
Dr. Wexler emphasized that the message from this study for healthcare providers and patients is clear. “Providers need to think about how they might redesign their system’s approaches with respect to patient care to find ways to implement these recommendations into the process in a way that is still efficient without negatively impacting patients or workflow,” said Dr. Wexler. “For patients, the study is a reminder of how important it is for them to pay attention to BP measurements and understand the proper process to take the measurement, including the AHA guidelines for in-clinic as well as out-of-clinic at home BP measurement. If they have questions, they should have a conversation with their provider.”
The CORRECT BP study was funded by Midmark but independently executed by non-affiliated research scientists and clinicians in conjunction with The Ohio State University to help ensure that “Good Clinical Practice Guidelines” were followed. The authors of the study are Bruce S. Alpert, Joseph E. Schwartz, Mira Shapiro and Randell K. Wexler.
Midmark was not directly involved with decisions related to the study design, data collection, analysis or interpretation of the data. The authors of the study had full autonomy to design and administer the protocol they conceived to ensure all data was unbiased, factual and illustrative of actual clinical outcomes. The CORRECT BP study authors and study designers chose to use the Midmark 626 Barrier-Free Examination Chair to ensure proper participant positioning following AHA recommendations.

